Gingiva: Gingiva is the soft tissue covering that surrounds the teeth consisting of fibrous tissue which is continuous with the periodontial ligament and the mucosa covering the teeth.
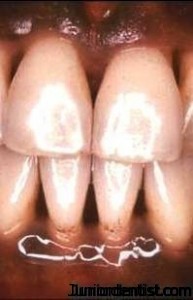
Gingiva shows stiplling, which is its typical appearance and is known as stippled gingiva as seen in the above picture.
The gingiva is a type of Masticatory mucosa.
 Gingiva is the soft tissue around the teeth which is continous with the Mucosa of the Oral cavity, this junction is called the mucogingival junction.
Gingiva is the soft tissue around the teeth which is continous with the Mucosa of the Oral cavity, this junction is called the mucogingival junction.
It is Differentiated by the line seen in the image which demarcates it due the dark color of the mucosa (due to high vasculature) and the light color of the gingiva (due to presence of more fibers) comparitively.
Gingival Sulcus: It extends from the gingival marging apically to the cemento-enamel junction, which acts as aseal against the tooth and acts as a barrier against the sub-gingival plaque, bacteria and prevents fluid loss from underlying tissue.
Gingiva is 75% Para Keratinized, 15% Keratinized and 10% non-keratinized.
Types:
The Gingiva is divided into:
- Attached Gingiva: The thick pink tissue that hugs the bone and is tightly attached to the underlying Bone and mucosa.
- Free Gingiva: The soft thin movable tissue that makes u the inside of the lips and cheeks.
Based on epithelium:
Oral Epithelium: It is a stratified squamous keratinizing epithelium, that lines the vestibular and oral surfaces of the gingiva it extends from the mucogingival junction to the gingival epithelium except for the palatal epithelium where it blends with the palatal epithelium.
Sulcular Epithelium: This is the epithelium which covers the gingiva present in the sulcus depths.
Junctional Epithelium: The portion of the gingival tissue that is attached the gingival connective tissue on one side and the tooth surface on the other. And its coronal end lines the end of gingival sulcus.
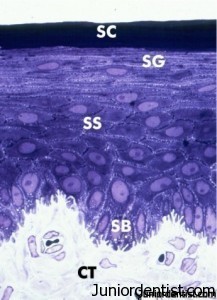
Histology: The gingiva is covered with Keratinized Stratified squamous epithelium the outer most layer of gingiva. This epithelial layer shows projections into the underlying Connective tissue which are known as “Rete Pegs”.
The outer layers of the epithelium are keratinized and are stratified so the size of the cells increases as we go into the gingiva.
The epithelium has 4 layers:
SC: Stratum Corneum-The cells are flattened, outermost layer.
SG: Stratum Granulosum-The cells contain granules and are relatively bigger in size
SS: Stratum Spinosum-The cells are spinous in appearance.
SB: Stratum Basale-The cells are rounded and these are the proliferative cells which give rise to new cells.
There is the connective tissue underneath the Epithelium which contains fibers, Blood vessels etc.
Cells: The different types of cells which are present in the Gingiva apart from the normal epithelial cells are
Melanocytes: They are the cells which give the darkish color of gingiva in some individuals which are dark skinned.
Langerhan Cell: These are the modified macrophages which help in producing antigens.
Merkel cell: these are present in the deep layers and act as tactile proprioceptive cells.
Fibers: The fibers are mainly
Collagen Fibers:
- Type VII collagen fibers are predominant which are present in intimate contact with basal lamina.
- Type IV collagen fibers present in basal linings of epithelial walls and blood vessels.
Elastin Fibers: Rare in lamina propria and common in lining mucosa, the elastic fibers are made up of
- Elastin: provide elastic nature
- Fibrillin:
Oxytalin Fibers: These resemble immature elastic fibers.
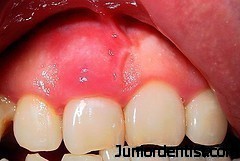
Gingival Diseases:
The gingival deiseases are mainly the inflamation of Gingiva which is known as Gingivitis, which is of 2 types
- ACUTE: It can be due to acute infections or due to poor oral hygiene and accumulation of plaque and calculus.
- CHRONIC: It is mainly caused due to Hormaonal imbalance, Poor Oral hygiene, Vitamin deficiency.

the contents given here are not up to the mark the should be re defined properly using standard books..
thanks
OralMax Gum Disease Treatment can help you with bleeding gums, inflammation, sensitivity and dental mobility.
Can help stop bone loss and reduce the dental mobility from grade 2 to grade 0 (Miller’s Classification).
All this thanks to the tannin acids (astringent) naturally obtained from different quercus species evaluated and recognized as an effective substance against bleeding gums, inflammation and dental mobility in diabetic and non-diabetic patients.
i have read only one topic and i liked that………………………..
well sorry but let me correct
type 1 and type 3 collagen are present in the ratio of 7:1
type 4 may be present…………
@Niraj will surely look into it and correct it with the correct information, thanx for correcting
Bleeding gums are mainly due to inadequate plaque removal from the teeth at the gum line. This will lead to a condition called gingivitis, or inflamed gums. If plaque is not removed through regular brushing and dental appointments, it will harden into what is known as tartar. Ultimately, this will lead to increased bleeding and a more advanced form of gum and jawbone disease known as periodontitis.`’-,
My web page
<http://wellnessdigest.co
The etiology, or cause, of plaque-induced gingivitis is bacterial plaque, which acts to initiate the body’s host response. This, in turn, can lead to destruction of the gingival tissues, which may progress to destruction of the periodontal attachment apparatus.`–`